All What You Need To Know About Pneumococcal Disease
Pneumococcal disease is a widespread problem, yet little is known about it. Despite the fact that millions of people are affected, this disease is unfairly overlooked thus explaining why reliable information about it is scarce. It’s time to change that! Throughout this article, you’ll learn more about the pneumococcal disease, its causes, symptoms, and so much more.
Pneumococcal disease overview and cause
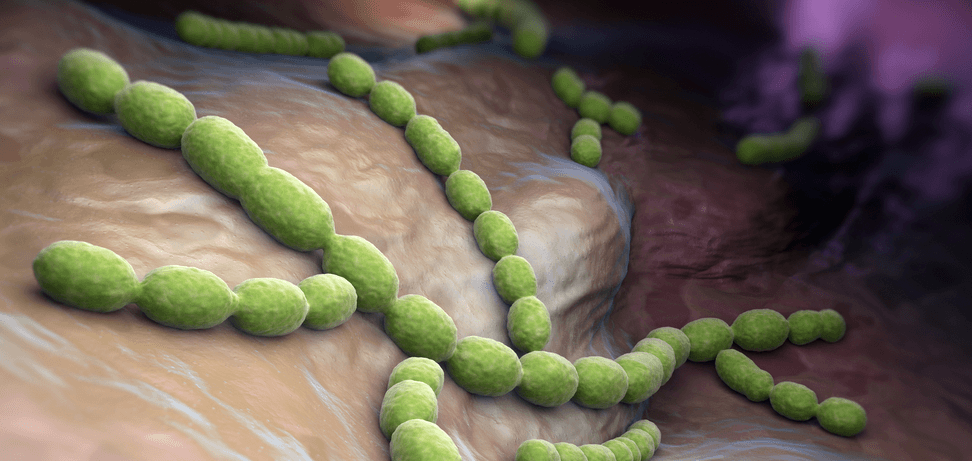
Pneumococcal disease is defined as an infection induced by Streptococcus pneumoniae bacterium, also called pneumococcus. The pneumococcus is the classic gram-positive extracellular pathogen. Evidence shows this bacterium is a major cause of mortality and morbidity on a global scale as it contributes to more deaths than any other infectious disease.
Pneumococcus or S. pneumoniae bacterium is a common inhabitant of the bacterial flora that colonizes nose and throat of both adults and children. It is estimated that 5% to 40% of the general population has this bacterium in the nasopharyngeal mucosa due to the surface adhesin protein which enables the bacteria to bind to epithelial cells. The most common carriers of these bacteria are children younger than six. While S. pneumoniae is a part of the normal microflora in the respiratory tract, it can cause diseases and infections due to its invasive nature. This bacterium can cause a wide array of problems, and some of them can be severe and life-threatening. These problems include pneumonia, bloodstream infections, ear and sinus infections, and bacterial meningitis.
How common is the pneumococcal disease?
As mentioned above, millions of people have the pneumococcal disease, and it’s time to provide more specific info. Estimates show that pneumococcal disease is the world’s #1 vaccine-preventable cause of death among infants and children younger than five. The CDC reports that S. pneumoniae bacterium kills almost a million children under five each year. A vast majority of deaths caused by pneumococcus occur in developing countries.
According to the World Health Organization, S. pneumoniae is the most prevalent cause of community-acquired bacterial pneumonia in the adult population in the US and Europe. More precisely, the annual incidence of pneumococcal disease is between 10 and 100 per 100 000 population, figures show.
Types of pneumococcal disease
Not all cases of the pneumococcal disease are equal, and we can divide them into two major types: non-invasive and invasive. Above in the article, some infections caused by pneumococcus were mentioned, but in this section, you’re going to learn more about them.
Non-invasive pneumococcal diseases
In some cases, the infection caused by the S. pneumoniae bacterium does not occur inside the major organs and blood. These infections are classified as non-invasive because they are milder than their counterparts. The underlying mechanism is straightforward; the bacteria spread from nose and throat to the upper or lower respiratory tract where they can cause the following problems:
- Non-bacteremic pneumonia – occurs when pneumococcal infection affects lower respiratory tract but without reaching the bloodstream
- Otitis media – infection of the middle ear. This particular infection is indicated by middle ear inflammation, earache, swelling of the eardrum, and the buildup of fluid in the middle ear. In some cases, the eardrum is perforated meaning pus starts leaking into the ear canal
Invasive pneumococcal disease
Unlike non-invasive infections which don’t enter organs and bloodstream, invasive pneumococcal disease develops inside an organ or in a patient’s blood. Some of these invasive pneumococcal diseases include:
- Bacteremic pneumonia – a severe condition where 20% of patients develop bloodstream infection too. inflammation can affect just one, or both lungs
- Meningitis – an inflammation of mengines or membranes that surround spinal cord and brain. Although most meningitis cases are due to a viral infection, some people can develop this form of invasive pneumococcal disease due to bacterial and fungal infections too
- Sepsis (bacteremia) – the presence of bacteria in the blood, a potentially life-threatening complication of an infection
Who’s at risk of pneumococcal disease?
Generally speaking, everyone can develop a pneumococcal infection. However, some people are more likely to get infected than others. An effective way to lower the risk of pneumococcal disease is to learn as much as you can about risk factors. To help you out, these are the most common risk factors to bear in mind:
- Travellers who visit developing countries or spend time in crowded settings and in contact with children where the pneumococcal conjugate vaccine isn’t used routinely
- Children younger than 2
- Adults 65 or older
- Having a condition that weakens the immune system such as heart disease, diabetes, HIV/AIDS, and lung disease
- Smoking cigarettes
- Asthma
- Cerebrospinal fluid leak or cochlear implant
- Functional or anatomic asplenia (absence of normal spleen function)
The pneumococcal disease typically occurs in winter and early spring in some places, but in tropic regions, it’s active all year round. While infections are less common in countries where the pneumococcal conjugate vaccine is used routinely, they can still occur in settings such as childcare centers, nursing homes, and others.
Transmission
Transmission of pneumococcus bacterium is a consequence of a direct person-to-person contact through respiratory droplets. Additionally, transmission occurs via autoinoculation in people who carry the bacteria in the upper respiratory tract. The term autoinoculation refers to movement or transfer of microorganisms, in this case, the bacteria, from an initial focus of infection to another site in the body. Different factors such as season, crowding, the presence of upper respiratory infections or pneumococcal disease, influence the spread of these bacteria within a household or family. It is important to bear in mind that having these bacteria in the body doesn’t automatically lead to pneumococcal disease, but it is a risk factor.
Symptoms of the pneumococcal disease
Basically, symptoms of the pneumococcal disease vary from one type of infection to another. The most common symptoms include:
- Aches and pains
- Chills
- Fever
- Generally feeling unwell (malaise)
- Headache
- Sweat
Symptoms that are specific for middle ear infection include an earache, ear discharge, temporary hearing loss, vomiting, diarrhea, and fever.
On the other hand, signs, and symptoms of pneumonia involve muscle aches, fatigue, cough, fever, shortness of breath, chest pain, nausea, headache, and vomiting.
Meningitis is indicated by a headache, fever, coma (in some cases), seizures, stiff neck, nausea and vomiting, irritability, sleepiness, and others.
Bacteremia involves symptoms such as rapid breathing, rapid heart rate, headache, fever, and aches and pains.
How is pneumococcal disease diagnosed?
Diagnosis of pneumococcal disease can be difficult and microbiological proof of infection might not exist. Healthcare professionals can still find out whether a patient has the pneumococcal disease in many ways. It is of huge importance for patients to inform their doctors about all the symptoms they experience, even if they don’t consider them important. Failing to report some symptom can make the diagnostic process more difficult.
At the very beginning, the doctor will perform a physical exam such as listening to the patient’s chest with a stethoscope. Different tests can make diagnosis easier, but the choice of tests varies from one patient to another. The exact tests depend on your symptoms, but they usually involve blood pressure test, X-ray of the chest, and sample tests of blood, sputum, cerebrospinal fluid, joint fluid, lung aspirate, peritoneal fluid, and other specimens. The purpose of these tests is to rule out other conditions and make an accurate diagnosis.
How is pneumococcal disease treated?
After the infection has been diagnosed, the physician recommends a suitable treatment option. Treatment of pneumococcal disease doesn’t go by “one size fits all” rule, it depends on the type of infection, the severity of symptoms, and other factors. Non-invasive infections such as middle ear pain can be treated with antibiotics. Even bacterial pneumonia requires the antibiotics used for successful treatment. On the flip side, severe infections require intravenous administration of a solution that contains antibiotics.
In cases when the bacteria have become resistant to some antibiotics, the doctor may recommend a combination of different antibiotics. Patients who have serious infections may need to be hospitalized.
Prevention of pneumococcal disease
Although there is still a lot we need to learn about the pneumococcal disease, what we do know is that prevention is possible. Unlike some other diseases and infections, the pneumococcal disease doesn’t have tons of preventive measures. The most important prevention method is vaccination.
Vaccination is the very best way to prevent pneumococcal infection is to get vaccinated. The pneumococcal conjugate vaccine protects you from 13 types of these bacteria, and it can also prevent ear infections in some people. In addition, the pneumococcal polysaccharide vaccine exhibits protection against 23 types of bacteria Bear in mind that there are more than 90 kinds of these bacteria and there is no vaccine that protects the body from all of them. However, currently available vaccines do a good job of minimizing the risk of getting infected
If you haven’t received the vaccine and are planning the trip to developing countries, you can consider discussing the vaccination subject with the doctor, especially if you have an infant.
Conclusion
Pneumococcal disease affects millions in developing countries, but it’s still present in the US and Europe too. Symptoms vary depending on the infection. These diseases can be non-invasive and invasive or life-threatening. Seeing the doctor in a timely manner to report the symptoms you experience is the best option for a successful treatment.
